Spinal Muscular Atrophy: Understanding Causes and Progressive Weakness
Spinal Muscular Atrophy (SMA) is a formidable genetic condition characterized by the progressive weakening and wasting away of muscles. Far from being a single disorder, SMA encompasses a group of inherited neuromuscular diseases, each with its own specific characteristics regarding onset, severity, and life expectancy. For those grappling with the implications of this condition, understanding its fundamental causes and the wide array of
SMA symptoms is the first crucial step towards informed management and support.
What is Spinal Muscular Atrophy (SMA)? A Deeper Dive into its Origins
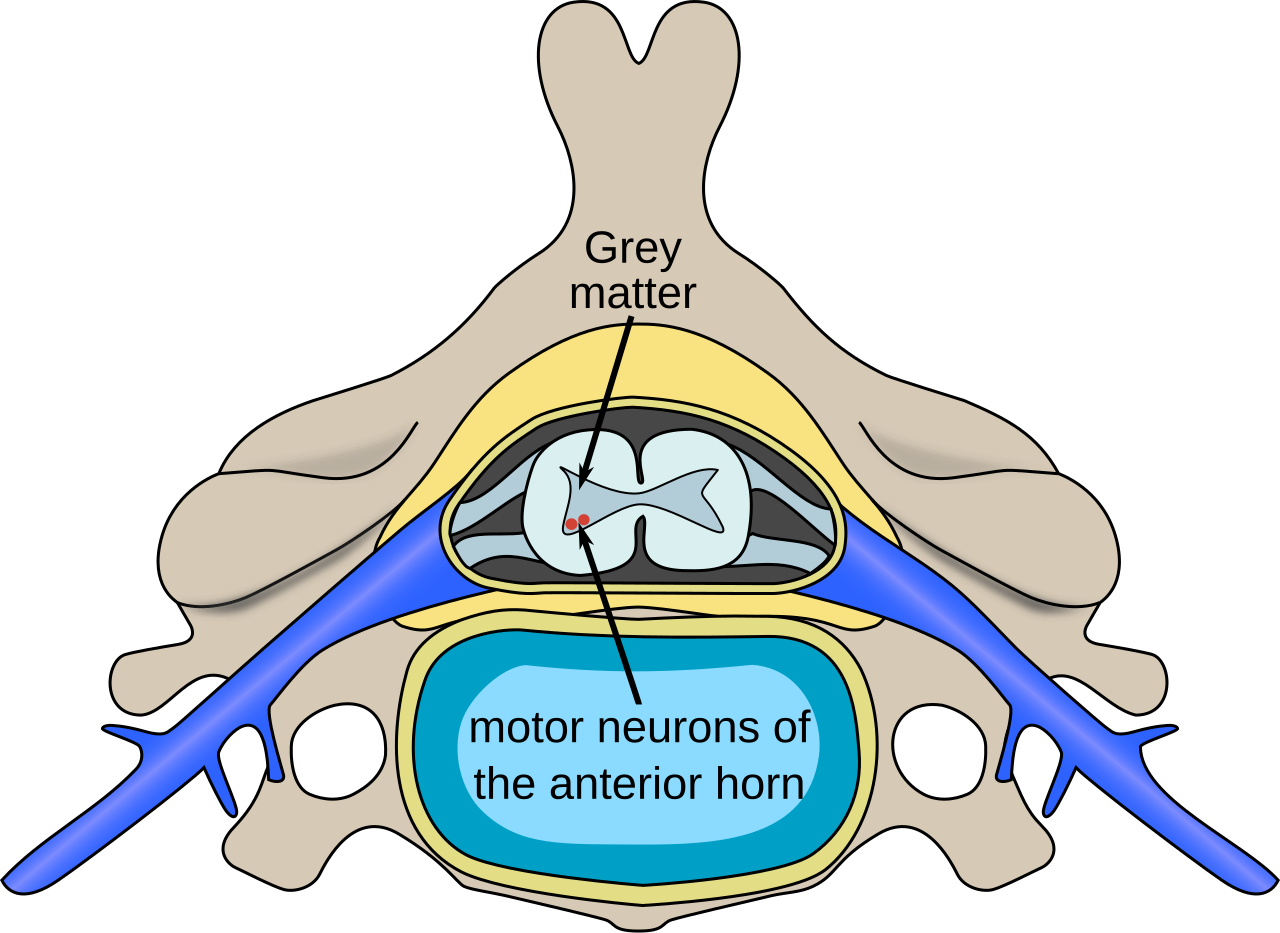
At its core, Spinal Muscular Atrophy is a disorder rooted in the loss of vital nerve cells within the spinal cord. Specifically, it targets the *lower motor neurons*, also known as *anterior horn cells* or *alpha-motoneurons*. These specialized nerve cells, located in the brainstem and the anterior horn of the spinal cord, are the direct communicators between your central nervous system and your muscles. Their primary function is to transmit the electrical impulses that initiate and control muscle movement – every step, every breath, every turn of the head depends on their healthy operation.
In individuals with SMA, these critical motor neurons progressively degenerate and die. Without these nerve cells functioning correctly, the muscles no longer receive the necessary signals to contract. This lack of innervation leads to muscle weakness and eventually, muscle atrophy (wasting away). The term "progressive" is key here, as the muscle weakness typically worsens over time, impacting mobility and vital bodily functions. Historically, the concept of progressive spinal muscular atrophy was notably defined by neurologist John Hoffmann in Heidelberg in 1893, laying foundational understanding for this group of disorders.
The weakness observed in SMA tends to be more pronounced in the *proximal muscles* – those closer to the center of the body, such as the shoulders, hips, and trunk – compared to the *distal muscles*, which are farther away (hands and feet). This proximal dominance can significantly impact core strength, sitting balance, and the ability to stand or walk.
Understanding "Sma Krankheit Symptome": The Core Manifestations
The overarching "Sma Krankheit Symptome" are centered around muscle weakness and hypotonia (decreased muscle tone). However, it's vital to recognize that the specific presentation and severity of these symptoms can vary dramatically, defining the different types of SMA. Healthcare providers classify SMA into five distinct subtypes (Type 0 through Type 4) based on several critical factors: the age when symptoms first appear, the overall severity of muscle weakness, and the expected life span. This classification helps in diagnosis, prognosis, and treatment planning.
While the primary "Sma Krankheit Symptome" involve generalized muscle weakness, especially in the core and limbs, secondary symptoms often arise due to this weakness. These can include difficulties with:
- Mobility: Challenges with crawling, sitting, standing, or walking.
- Breathing: Weakness of respiratory muscles can lead to shallow breathing, recurrent chest infections, and, in severe cases, respiratory failure.
- Swallowing and Feeding: Weakness in facial, throat, and tongue muscles can make eating and drinking difficult, leading to poor nutrition and aspiration risks.
- Skeletal Deformities: Progressive muscle weakness can lead to scoliosis (curvature of the spine) and joint contractures.
Understanding these varying manifestations is crucial for comprehensive care, as each type of SMA presents unique challenges and requires tailored interventions.
The Spectrum of Weakness: Exploring SMA Subtypes
The journey of SMA is not uniform; it unfolds differently across its various subtypes, each presenting a distinct clinical picture. Here’s a closer look at the five recognized types, highlighting the specific "Sma Krankheit Symptome" associated with each:
- SMA Type 0 (Congenital SMA): This is the rarest and most severe form, with symptoms manifesting even before birth. Decreased fetal movements are often noted pre-birth. Infants with Type 0 exhibit profound muscle weakness and hypotonia at birth, often leading to severe respiratory failure. Tragically, death usually occurs at birth or within the first month of life. The challenges of pre-birth diagnosis underscore the severity and rapid progression of this type.
- SMA Type 1 (Severe SMA / Werdnig-Hoffman Disease): Representing about 60% of all SMA cases, Type 1 is a severe form where SMA symptoms typically appear within the first six months of life. Infants struggle with significant hypotonia, limited head control, and an inability to sit without support. Crucially, they experience difficulties with swallowing and breathing, necessitating intensive respiratory and nutritional support. Without such support, children with Type 1 SMA often do not survive past their second birthday. Early diagnosis and intervention are paramount for improving quality of life and prolonging survival in these cases.
- SMA Type 2 (Intermediate SMA / Dubowitz Disease): Symptoms for Type 2 SMA typically emerge between six and 18 months of age. Children with this type develop hypotonia and progressive muscle weakness, which often affects their legs more significantly than their arms. While they may learn to sit independently, they generally cannot stand or walk without assistance. Respiratory issues become a major concern as the disease progresses, often being the primary cause of mortality. With modern care, around 70% of individuals with Type 2 SMA can survive into their 20s, and some into their 30s, emphasizing the importance of ongoing medical and rehabilitative support.
- SMA Type 3 (Mild SMA / Kugelberg-Welander Disease): This milder form of SMA sees symptoms appearing after 18 months of age, often not until early childhood or even adolescence. The primary manifestation is lower limb muscle weakness, leading to difficulties with walking, running, and climbing stairs. While individuals with Type 3 SMA may initially walk independently, they might lose this ability over time. Unlike more severe types, breathing issues are uncommon, and the condition typically does not affect life expectancy, allowing many to lead full, productive lives with appropriate physical therapy and adaptive aids.
- SMA Type 4 (Adult-Onset SMA): The mildest form, Type 4 SMA usually doesn't appear until after the age of 21. Muscle weakness progresses very slowly, primarily affecting proximal muscles in the limbs. Most individuals with Type 4 SMA retain their mobility throughout their lives and maintain a normal life expectancy. Diagnosis can sometimes be delayed due to the subtle and slowly progressing nature of the symptoms, often requiring careful neurological evaluation to differentiate it from other neuromuscular conditions. You can learn more about the specifics of these categories in The Five Types of SMA: Onset, Severity, and Life Expectancy Explained.
Managing Progressive Weakness: Current Approaches and Future Hopes
While there is currently no outright cure for SMA, significant advancements in therapies and medications have dramatically changed the landscape for individuals living with the condition. The goal of treatment is to manage "Sma Krankheit Symptome", slow disease progression, and enhance the quality of life.
Key management strategies include:
- Symptom-Modifying Therapies: Recent breakthroughs, particularly in gene therapy and RNA-modifying drugs, aim to address the underlying genetic defect, either by replacing the missing or faulty gene or by increasing the production of the survival motor neuron (SMN) protein that is deficient in SMA. These treatments have shown remarkable promise in improving motor function and extending survival, especially when initiated early.
- Rehabilitative Therapies: Physical and occupational therapy are crucial for maintaining existing muscle function, preventing joint contractures, improving range of motion, and teaching compensatory strategies. Speech therapy can assist with swallowing difficulties and communication.
- Respiratory Support: For individuals with compromised breathing, interventions may range from non-invasive ventilation (e.g., BiPAP) to mechanical ventilation, along with devices like cough assist machines to help clear airways and prevent infections.
- Nutritional Support: Managing feeding difficulties through modified diets, feeding tubes, or other nutritional interventions is essential to ensure adequate growth and energy for those affected.
- Orthopedic Management: Regular monitoring for scoliosis and other skeletal issues, along with bracing or surgical interventions when necessary, can help maintain spinal alignment and comfort.
- Psychosocial Support: Addressing the emotional and social impacts of SMA for patients and their families is vital. Support groups, counseling, and mental health services play a significant role.
The landscape of SMA treatment is rapidly evolving, offering renewed hope. Ongoing research continues to explore new therapeutic avenues, aiming for even more effective ways to combat the progressive weakness and improve the lives of those affected by Spinal Muscular Atrophy.
Conclusion
Spinal Muscular Atrophy is a complex genetic condition defined by the progressive loss of motor neurons, leading to muscle weakness and atrophy. Understanding the diverse "Sma Krankheit Symptome" and the unique characteristics of its five subtypes is essential for early diagnosis, appropriate intervention, and comprehensive care. While the journey with SMA presents significant challenges, advancements in therapies, coupled with dedicated supportive care, are continually improving outcomes and enhancing the quality of life for individuals across the spectrum of this condition. Continued research holds the promise of even more effective treatments and, ultimately, a brighter future for those affected by SMA.